Firefighters facing exceedingly high levels of occupational cancers

In January this year, the Montreal Firefighters Association released a call to expand the list of cancers that are recognized as occupational diseases for firefighters – a move that firefighters’ associations around Canada are in total support of.
According to a study conducted by the University of Fraser Valley in B.C., 86 per cent of firefighter line of duty deaths in Canada are attributable to cancer. Firefighters, by virtue of the job that they do, are typically in excellent physical condition. “However, when it comes to cancers, [firefighters] far exceed the general public,” says Neil McMillan.
McMillan is an elected executive member with IAFF Local 162 in Ottawa. He is chair of the WSIB committee for the local association, which covers around 1,000 unionized firefighters in Ottawa.
“The issue of occupational disease is rampant within the fire service. Unfortunately, we’re struck down at very high rates of certain illnesses, and specifically cancers as well as cardiovascular disease, and those systems that are regulated through our endocrine systems like our reproductive tracts.”

Martin Charbonneau. Died of cancer March 9th, 2021. He was 49 years old, and his claim remains denied by WSIB. He left behind a widow and two children.
Harvesters of carcinogens
Firefighters face a number of risks, the contents of a home when it burns produces all sorts of chemical exposures. They also face potential exposures within their fire stations, and exposures to equipment that have different toxins in them.
While firefighters may accept that there are some inherent risks to their occupation, a lot of exposures that come from their workplace are unnecessary.
“We are harvesters and depositors of carcinogens. The studies that have been done in fire stations, fire station dust and fire station air sampling have shown that we’ve taken all these products of combustion, all these heavy metals, all these know carcinogens, and brought them back to our place of employment. Trying to eliminate those unnecessary exposures are things we need to be cognizant of,” says McMillan.
And the science has changed over time with the development of firefighter PPE. Prior to the age of self-contained breathing apparatus, a lot of the exposures firefighters received from smoke were assumed to be inhalation exposures. As such, initial legislation presumptions reflected that with lung cancer and mesothelioma. However, McMillan says that what they find through modern research is that the dermal absorption of smoke and particulate aerosolized products and gases are a real risk.

Ryan Hill. Died Dec. 20th, 2021, a day after his 37th birthday. His cancer claim is yet to be approved by WSIB due to policy limitations, despite it being a presumptively recognized cancer for firefighters. He left behind a young widow and twin 4 year old boys.
In addition, recent studies from California show female firefighters are exposed to higher levels of certain PFAS chemicals, as compared to other workers, which are found within the foam that firefighters use, and the Bunker gear meant to protect them. There are a host of risks associated with PFAS exposure, not only are they carcinogens but they are endocrine-disrupting chemicals which are very bio persistent. Indeed, some PFAS chemicals can sometimes have a half life of nine years.
“Female firefighters are a small cohort among the overall firefighting population which makes it them difficult to study,” says McMillan. Their high rates of exposures have an effect on cancer rates and reproductive and cardiovascular disease as well as reproductive effects, and in Ontario there is “a disparity on presumptive coverage for reproductive tract cancers for female firefighters; male reproductive tracts are covered,” he says.
Presumptive coverage
In Ontario, firefighters have (rebuttable) presumptive coverage for 17 types of cancers as well as cardiac events such as myocardial infarction or a heart attack within 24 hours of a fire event. Presumptive coverage varies throughout Canada (e.g. in Manitoba there is presumptive coverage for 19 types of cancers). And there are caveats and criteria associated with these.
“And then there’s the years of service or durations of employment that are also included which are ill-defined through the policy. It’s resulted, in Ottawa, in a lot of our members who have cancers that are designated as presumptive cancers that are not getting covered because some of these other criteria disqualify them.”
McMillan’s association, under the leadership of Local 162 President Doug McLennan, has recently decided to align itself with Ontario’s Occupational Disease Reform Alliance (ODRA). “The asks that they’re making are wholly applicable to some of the barriers and challenges that our firefighters have faced in their claims adjudication with WSIB.”
He says that occupational exposures are top priority within the association, “because of the effects it has on our members and the families and communities. Securing entitlements and benefits and reducing the incidences of debilitating and often fatal diseases is a core mission of our Association, supported by President McLennan on down.”
Inconsistent policies
McMillan and his colleagues are currently dissatisfied with the rate of claims accepted by WSIB which he says is just too low.
“There needs to be changes to allow for our members’ occupational illnesses to be accepted by WSIB. I think that the application of WSIB policies has been inconsistent. I would like to see a higher percentage of acceptances or firefighter cancer claims, as supported by current advances in scientific research.”
The burden of proof is simply too high, and criteria within policies are too stringent.
For example, in the instance of colorectal cancer, if the diagnosis occurs after age 61, it no longer fits within the policy. The cut off point seems almost arbitrary despite the fact that latency periods are not an exact science, they’re more of a bell curve, as aptly illustrated by Dr. Paul Demers in his report to WSIB in 2020. To assign a specific date or number of years of service to be eligible discounts the fact that other synergistic exposures within the workplace can shift latency and carcinogenesis depending on somebody’s frequency and duration of exposures, says McMillan.
“There’s a very rigid application within WSIB that doesn’t account for that. There’s a great divide as to how these policies are enacted, and the spirit in which they were written,” he says.
Decisions should be being made to a degree of reasonable medical probability as to whether the workplace contributed in part to the illness, with the benefit of the doubt siding with the worker as prescribed by the Act (WSIA). When opinions are being asked from some compensation boards’ ‘subject matter experts’ it should be leaning more towards that as opposed to causative certainties.
In addition, some of these occupational medical consultants have financial interests in the opinions they provide, says McMillan. “I’ve seen some of these individuals who hold board positions in for-profit companies that market themselves to industry to ‘reduce exorbitant workers’ compensation costs for businesses.”
And their evidence is placed higher than evidence provided by treating practitioners that see, touch and treat the patients and don’t have a vested interest in injured workers.
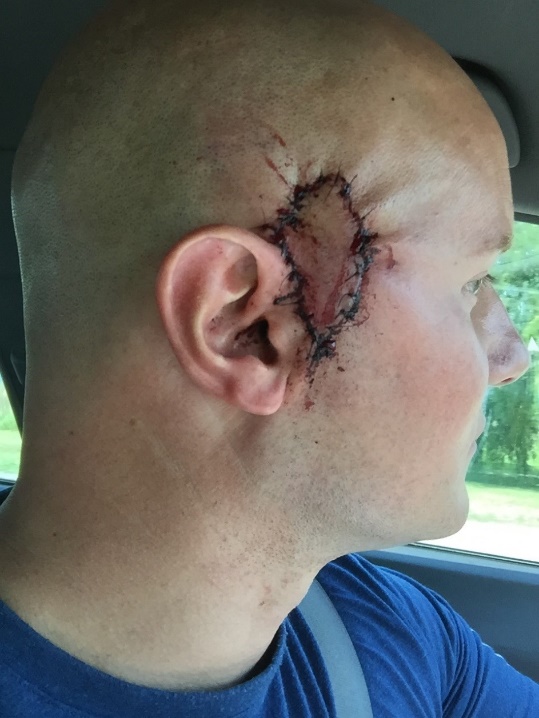
McMillan: “I went straight from work to the hospital to have an invasive malignant melanoma excised from my right temple in 2016. I was 37 years old, and had 13 years of firefighting tenure. My cancer is one of the presumptively covered cancers, but I required 15 years of service to receive recognition, and as such my claim remains denied.”
“I find that the principles of merits and justice, and benefit of the doubt for the worker, are not being considered appropriately in many claims by WSIB, when they can have one medical consultant who is a physician in occupational medicine whose opinion is greater than subject matter experts on those specific illnesses, it shifts a burden of proof on workers in excess of what the WSIA requires.
To have individuals who claim to have an expertise in occupational medicine say they don't believe that these risks are there, even though universities across North America, Europe and Australia have proven otherwise, makes me know that I have a lot more work to do in the future,” says McMillan.
No recognition
McMillan says that these claims that are denied are a disservice to firefighters and their families. “It’s unfortunate that our members who, in the service of their community, are doing the job that was asked of them and are covered in soot and coughing up black for days after a fire don’t receive the recognition that they deserve.”
The lack of compensation denotes a lack of recognition for the occupational risks that firefighters are exposed to during the course of their work – hazards that all too often they simply can’t avoid.
Says McMillan: “When the bells ring and we go to a fire, we’re happy to put ourselves in harm’s way only with the hope that if we do take ill as a result of it years later, that we’ll receive some type of compensation for ourselves and our families.”





